DEFINING COMPLEX ADHD
Complex ADHD is more the norm than the exception1
Once considered a simple disorder, ADHD is now known to have multifaceted manifestations, leaving many patients vulnerable to psychiatric comorbidities.1-4
ADHD Knowledge Has Grown
The way we understand ADHD in pediatric patients has changed into something more complex1-3
ADHD was once viewed as either a discrete behavioral condition or a secondary one1-3
While ADHD symptoms may be present in other neuropsychiatric conditions, ADHD is often the first disorder to appear. The following comorbidities tend to develop later2:
- Depression
- Anxiety disorders
- Conduct disorders
Such sequencing of symptoms has led some to suggest that executive functioning deficits in individuals with ADHD may leave them more vulnerable to future psychiatric illness, and therefore should be monitored for any symptoms.
ADHD carries a significant burden of illness—particularly in the presence of comorbidities2
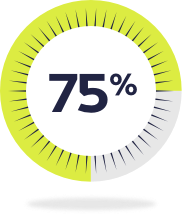
Up to 75% of pediatric patients with ADHD have a comorbid psychiatric condition4-6

And approximately 60% have multiple psychiatric comorbidities.4-6
Incidence and Definition of Complex ADHD
It’s important to understand the intricacies of complex ADHD
While a certain proportion of children with ADHD express symptoms of ADHD alone (often described as “simple ADHD”), we now know that this is overwhelmingly the exception rather than the norm.1-3
ADHD is now thought to be a complex genetic trait with a heterogenous presentation based upon a phenotype ranging from mildly to severely affected.7
ADHD is one of the most common neurodevelopmental disorders8
The prevalence of ADHD in children in the United States is approximately 9-11%.9-12
Research also points to ADHD as an impairment of executive function that negatively impacts the brain’s cognitive architecture.2 This has far-reaching consequences in the domains of:
School/education
Home/family life
Emotional development
Peer interaction
It is important that parents of children with ADHD understand these complexities in order to set appropriate expectations for their child’s treatment plan.
Key Takeaways
- ADHD is often present in other neuropsychiatric conditions4,5
- ADHD is often the first disorder to appear2
- ADHD is a complex genetic trait7
Stay in the know and access an exclusive ADHD resource

“Unmasking ADHD” can help you differentiate between ADHD and the most common overlapping comorbidities in children.
UP NEXT:
REFERENCES
- Koolwijk I, Stein DS, Chan E, Powell C, Driscoll K, Barbaresi WJ. “Complex” attention-deficit hyperactivity disorder, more norm than exception? Diagnoses and comorbidities in a developmental clinic. J Dev Behav Pediatr. 2014;35:591-597.
- Brown TE. Developmental complexities of attentional disorders. In: Brown TE, ed. ADHD Comorbidities: Handbook for ADHD Complications in Children and Adults. Arlington, VA: American Psychiatric Publishing Inc; 2009:3-23.
- Shaw P, Polanczyk GV. Combining epidemiological and neurobiological perspectives to characterize the lifetime trajectories of ADHD. Eur Child Adolesc Psychiatry. 2017;26(2):139-141.
- Banaschewski T, Becker K, Dopfner M, Holtmann M, Rosler M, Romanos M. Attention-deficit/hyperactivity disorder. Dtsch Arztebl Int. 2017;114(9):149-159.
- Reale L, Bartoli B, Cartabia M, et al. Comorbidity prevalence and treatment outcome in children and adolescents with ADHD. Eur Child Adolesc Psychiatry. 2017;26(12):1443-1457.
- Hervás, de Santos T, Quintero J, et al. Delphi Consensus on Attention Deficit-Hyperactivity Disorder (ADHD): evaluation by a panel of experts. Actas Esp Psiquiatr. 2016;44(6):231-243
- Acosta MT, Arcos-Burgos M, Muenke M. Attention deficit/hyperactivity disorder (ADHD): complex phenotype, simple genotype? Genet Med. 2004;6(1):1-15.
- Centers for Disease Control and Prevention. What is ADHD? https://www.cdc.gov/ncbddd/adhd/facts.html. Accessed April 14, 2021.
- Kessler RC, Adler L, Barkley R, et al. The prevalence and correlates of adult ADHD in the United States: results from the National Comorbidity Survey Replication. Am J Psychiatry. 2006;163(4):716-723.
- Merikangas KR, He JP, Burstein M, et al. Lifetime prevalence of mental disorders in US adolescents: results from the National Comorbidity Survey Replication--Adolescent Supplement (NCS-A). J Am Acad Child Adolesc Psychiatry. 2010;49(10):980-989.
- Visser SN, Danielson ML, Bitsko RH, et al. Trends in the parent-report of health care provider-diagnosed and medicated attention-deficit/hyperactivity disorder: United States, 2003-2011. J Am Acad Child Adolesc Psychiatry. 2014;53(1):34-46.e32.
- Fayyad J, Sampson NA, Hwang I, et al. The descriptive epidemiology of DSM-IV adult ADHD in the World Health Organization World Mental Health Surveys. Atten Defic Hyperact Disord. 2017;9(1):47-65.


