COMPLEX ADHD IN ADULTS
ADHD is a complex disorder in adults1
Diagnosis and treatment of adult ADHD are made challenging by the neuropathology underlying the disorder, as well as the prevalence of psychiatric comorbidities.1-4
Defining Complex ADHD
ADHD is now thought to be a complex genetic trait with a heterogenous presentation based upon a phenotype ranging from mildly to severely affected5
Adult ADHD carries a profound functional and psychosocial burden—particularly in the presence of comorbidities.2
ADHD has been found to be associated with an elevated all-cause mortality risk.6
- This risk increases with later age of diagnosis, in adulthood, and when comorbid conditions are present6
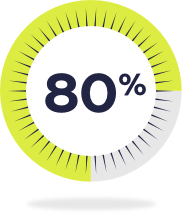
Up to 80% of adult patients with ADHD may have a comorbid psychiatric condition.2
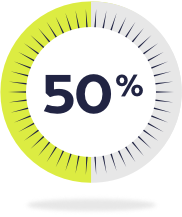
And over 50% may have multiple psychiatric comorbidities.7
The most common include2,4:
- Substance use disorder
- Mood disorders (eg, bipolar disorder, depression, dysthymia)
- Anxiety disorders
- Phobias
These comorbidities present significant clinical challenges, since their co-occurrence is linked to more severe illness course than ADHD or psychiatric disorders alone.2
Research has also shown that adults with ADHD are twice as likely to attempt suicide and 6 times as likely to complete it8:
- Men and women with ADHD appear to be equally impacted by suicidality9
- The financial distress often associated with adult ADHD has been implicated as a causal factor, conferring a 4-fold greater risk for suicide9
Early and optimal treatment of ADHD therefore has the potential to lessen overall disease burden for patients by preventing the emergence of psychiatric comorbidities, including suicide.2,9
Adult ADHD has also been strongly linked to somatic disorders10
- It is most consistently associated with greater risk for obesity, sleep disorders, asthma, migraine, and celiac disease10
- It is less robustly, though still notably, associated with greater risk for irritable bowel syndrome, restless leg syndrome, and chronic fatigue10
Neurobiology of Adult ADHD
Studies have demonstrated a multifactorial causality underlying both the expression and severity of ADHD in adults1,11
The pathogenesis of ADHD is complex, involving an interplay of genes and environment5,12-14
Affected brain regions in adult ADHD include:
1. Dorsal Anterior Cingulate Cortex
Plays a key role in cognitive, motor, and emotional processing; may fail to activate in adults with ADHD, leading to cognitive deficits11,15
2. Prefrontal Cortex
Linked to complex thought and working memory; cortical thickness has been found to be reduced in patients with adult ADHD11,14
3. Ventromedial Prefrontal Cortex
Modulates complex decision-making and strategic planning; blood flow to the frontal cortex shown to be impaired in adults with ADHD11,15
Neurotransmitter circuits are also involved in adult ADHD, and include the11:
Dopaminergic system11
Plays a key role in the planning and initiation of motor responses, activation, and reward seeking.
Noradrenergic system11
Influences arousal and cognitive processing of urgent stimuli
In adults with ADHD, dopaminergic pathways of the frontal-striatal circuitry may be dysfunctional, particularly during cognitive tasks.14,15
For a more detailed look at ADHD, download The Neurobiology of ADHD White Paper
Key Takeaways
- A primary diagnosis of ADHD may predispose adults to future psychiatric issues, including increased risk for suicide2,9
- Dysregulation in both brain regions and neurologic pathways is seen in adults with ADHD11,15
UP NEXT:
REFERENCES
- Volkow ND, Swanson JM. Adult attention-deficit disorder. N Engl J Med. 2013;369(20):1935-1944.
- Katzman MA, Bilkey TS, Chokka PR, Fallu A, Klassen LJ. Adult ADHD and comorbid disorders: clinical implications of a dimensional approach. BMC Psychiatry. 2017;17:302.
- Anker E, Bendiksen B, Heir T. Comorbid psychiatric disorders in a clinical sample of adults with ADHD, and associations with education, work, and social characteristics: a cross-sectional study. BMJ Open. 2018;8:e019700. doi: 10.1136/bmjopen-2017019700.
- Tsai F-J, Tseng W-L, Yang L-K, Gau SS-F. Psychiatric comorbid patterns in adults with attention-deficit hyperactivity disorder: treatment effect and subtypes. PLoS ONE. 2019;14(2):e0211873.
- Acosta MT, Arcos-Burgos M, Muenke M. Attention deficit/hyperactivity disorder (ADHD): complex phenotype, simple genotype? Genet Med. 2004;6(1):1-15.
- Sun S, Kuja-Halkola R, Faraone SV, et al. Association of psychiatric comorbidity with risk of premature death among children and adults with attention-deficit/hyperactivity disorder. JAMA Psychiatry. 76(11):1141-1149.
- Clemow DB, Bushe C, Mancini M, Ossipov MH, Upadhyaya H. A review of the efficacy of atomoxetine in the treatment of attention-deficit hyperactivity disorder in children and adult patients with common comorbidities. Neuropsychiatr Dis Treat. 2017;13:357-371.
- Faraone SV, Banaschewski T, Coghill D, et al. The World Federation of ADHD International Consensus Statement: 208 evidence-based conclusions about the disorder. Neurosci Behav Rev. Preprint posted online February 4, 2021. doi: 10.1016/j.neubiorev.2021.01.022.
- Beauchaine TP, Ben-David I, Bos M. ADHD, financial distress, and suicide in adulthood: a population study. Sci Adv. 2020;6(40):eaba1551. doi: 10.1126/sciadv.aba1551.
- Instanes JT, Klungsøyr K, Halmøy A, Fasmer OB, Haavik J. Adult ADHD and comorbid somatic disease: a systematic literature review. J Atten Disord. 2018;22(3):203-228.
- Faraone SV, Asherson P, Banaschewski T, et al. Attention-deficit/hyperactivity disorder. Nat Rev Dis Primers. 2015;1:1-23.
- Banaschewski T, Becker K, Dopfner M, Holtmann M, Rosler M, Romanos M. Attention-deficit/hyperactivity disorder. Dtsch Arztebl Int. 2017;114(9):149-159.
- Shadrin AA, Smeland OB, Zayats T, et al. Novel loci associated with attention-deficit/hyperactivity disorder are revealed by leveraging polygenic overlap with educational attainment. J Am Acad Child Adolesc Psychiatry. 2018;57(2):86-95.
- Kooij JJS, Bijlenga D, Salerno L, et al. Updated European Consensus Statement on diagnosis and treatment of adult ADHD. Eur Psychiatry. 2019;56:14-34.
- Matas M. Approach to attention-deficit disorder. Can Fam Physician. 2006;52(8):961-964.